Symptoms of Hypothyroidism: The Complete 2025 Guide
Table of Contents
- What Hypothyroidism Feels Like
- Understanding Hypothyroidism
- Complete Symptom List
- Environmental Causes
- Testing & Diagnosis
- Treatment Options
- Order Testing
What Hypothyroidism Actually Feels Like: The Brutal Truth
If your thyroid isn’t working properly, it has a tendency to make you feel like you were hit by a car the previous day.
Just imagine this perfect storm of misery:
- Tired beyond comprehension (not “I need coffee” tired—”I could sleep standing up” tired)
- Emotional for no apparent reason
- Depressed despite having nothing to be depressed about
- Overweight no matter what you eat or how much you exercise
- Hair falling out in alarming quantities (professional drain clogger status)
- Constipated to the point of contemplating a second mortgage for fiber supplements
- Hands and feet always freezing (ask my wife—it’s not charming)
- Brain feels like mush (trying to think through mental fog thicker than pea soup)
Undiagnosed hypothyroidism is not a pretty picture. Believe me.
The good news is that it’s usually straightforward to diagnose with lab tests, and treatment regimens can more or less turn you back into a normally functioning, healthy human being. The emphasis here is on “diagnosed”—which 10 million Americans haven’t achieved yet.
What Is Hypothyroidism? Understanding Your Thyroid’s Failure
Hypothyroidism occurs when your thyroid gland doesn’t make enough thyroid hormones—specifically T3 (triiodothyronine) and T4 (thyroxine)—to help regulate most of your body’s functions.
To put this in perspective: T3 regulates the metabolic rate of EVERY SINGLE CELL in your body [2]. When you don’t have enough, every cell in your body is essentially working at half-speed.
It’s like trying to run a computer with 5% battery power. Sure, it technically still works, but everything is painfully slow and barely functional.
The Epidemic Nobody’s Talking About
Currently, it’s estimated that 20 million Americans have some form of thyroid disease.
According to The American Association of Clinical Endocrinologists, half of people who suffer from thyroid disorders—10 million Americans—are currently undiagnosed [1].
Let that sink in. 10 million people walking around feeling like absolute garbage, and they don’t even know why.
Why So Many Undiagnosed Cases?
Lack of awareness. Plain and simple.
Many people don’t associate “feeling like crap” with “disease.” They think:
- “I’m just getting older”
- “I need to exercise more”
- “I’m probably just stressed”
- “Everyone’s tired these days”
Medical practitioners often overlook or misdiagnose hypothyroidism symptoms as:
- Normal aging (especially in patients over 60)
- Depression (prescribe antidepressants, miss the root cause)
- Stress or burnout
- “Non-illness” causes (i.e., “You just need to sleep more and eat better”)
The end result? People don’t recognize their symptoms as hypothyroid, and so they slog through every day tired, often depressed, and struggling with a host of other associated conditions—for years or even decades.
The Good News About Hypothyroidism (Yes, There Really Is Good News)
Dr. Amy Myers is a current tour de force expert on thyroid disease and has pioneered treating it from a functional perspective. In her book, aptly named The Thyroid Connection, Myers highlights in glaring detail that untreated thyroid disease takes over your life.
As in, it affects your:
- Work performance (brain fog makes complex tasks nearly impossible)
- Relationships (depression and irritability strain even strong bonds)
- Ability to parent effectively (exhaustion leaves nothing for your kids)
- Mental health (the thyroid-depression connection is profound)
- Physical health (every system in your body suffers)
- Overall quality of life (it’s hard to enjoy anything when you feel this bad)
“Takes over your life” = “feel crummy all the time.”
But here’s the hopeful part: Myers’s book (along with her other programs) shows in great detail that despite how much thyroid disease symptoms can negatively impact daily functioning, you have every reason to live a completely normal, healthy life.
Why There’s Real, Tangible Hope
The good news about hypothyroidism is that the road to health from a diagnosis can happen extremely quickly and dramatically.
Within weeks of starting proper treatment, many people report:
- Energy returning (sometimes dramatically)
- Brain fog lifting (like someone turned the lights back on)
- Mood stabilizing (depression that wouldn’t respond to antidepressants suddenly lifts)
- Weight beginning to normalize (metabolism finally works again)
- Hair loss stopping (and regrowth beginning)
Reversing hypothyroidism symptoms is not all fun and games—it requires dedication to treatment, lifestyle changes, and often addressing root causes. But it’s extremely achievable with evidence-based medicine (both conventional and functional) and sustainable life changes.
In fact, many people come out on the other end of their thyroid journey healthier than they were before diagnosis. Sometimes a health crisis becomes the catalyst for overall wellness transformation.
But first, you absolutely must get diagnosed. And that starts with recognizing the symptoms and ordering comprehensive testing.
What Is the Thyroid and What Does It Do?
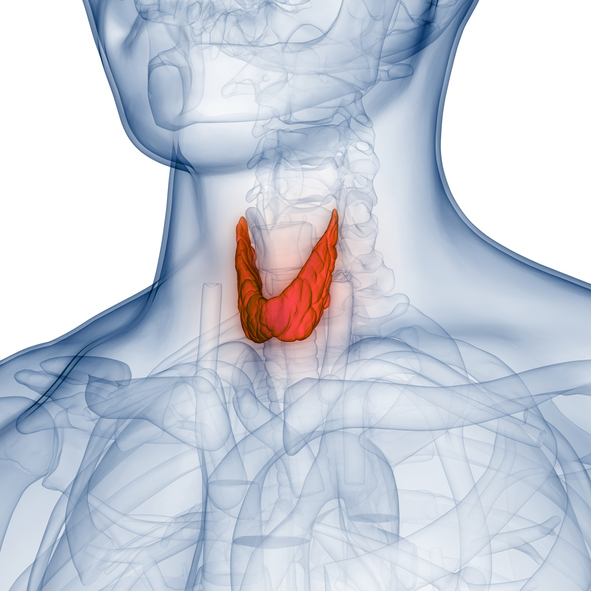
It’s difficult to overestimate just how important this little butterfly-shaped gland is.
Location and Size
Your thyroid sits right below your Adam’s apple, in front of your trachea (windpipe). If it’s healthy, you’ll never even know it’s there because you won’t be able to feel it.
It weighs less than an ounce. This tiny gland—smaller than a plum—controls your entire metabolism.
The Thyroid’s Wide-Ranging Duties
Just some of the critical functions your thyroid regulates:
- Regulate hormones throughout your body
- Regulate metabolism (how fast your cells burn energy)
- Influence growth and development (critical in childhood, important in adults)
- Regulate temperature (your internal thermostat)
- Help organs work efficiently (heart, brain, liver, kidneys—all of them)
As one person recently put it: “When the thyroid doesn’t work, everything gets out of whack.”
“Out of whack” is actually a perfect way to describe the feeling of untreated thyroid disease. It’s not one specific thing that’s wrong—it’s everything feeling slightly (or significantly) off.
How the Thyroid Works: The Gas Pedal System
Layman’s Description:
The hypothalamus, pituitary, and thyroid work together to maintain healthy hormone levels through a feedback loop system.
Think of it like a car:
- The hypothalamus is the driver monitoring speed
- The pituitary gland is the gas pedal
- The thyroid is the engine
When thyroid hormone levels are LOW:
- The hypothalamus notices and tells the pituitary
- The pituitary steps on the gas pedal (produces TSH)
- The thyroid produces more hormone using iodine
When thyroid hormone levels are HIGH:
- The hypothalamus notices and signals the pituitary
- The pituitary takes the foot off the gas pedal (reduces TSH)
- The thyroid produces less hormone
In hypothyroidism, the pituitary is flooring the gas pedal, but the engine (thyroid) can’t produce enough power.
More Technical Description (For the Science Nerds)
Your thyroid works via the hypothalamic-pituitary-thyroid axis (HPT axis).
The feedback loop:
- Hypothalamus monitors thyroid hormone (T3/T4) levels in blood
- If levels are low, hypothalamus releases TRH (thyrotropin-releasing hormone)
- TRH stimulates pituitary gland to produce TSH (thyroid-stimulating hormone)
- TSH stimulates thyroid to produce more T3 and T4 (using iodine)
- If pituitary doesn’t produce TSH (because T3/T4 levels are adequate), thyroid reduces production
Hypothalamus (monitors T3/T4) → TRH → Pituitary (controls production) → TSH → Thyroid (produces T3/T4)
When this system breaks down at the thyroid level, you get hypothyroidism.
Common Symptoms of Hypothyroidism: How to Recognize Thyroid Disease
Like any illness or disease, every person with hypothyroidism will experience a different combination of symptoms. The keywords here are combination and characterize.
We all experience tiredness, coldness, weight gain, and the other symptoms listed below occasionally. That’s normal human existence.
Quick Self-Assessment: Could You Have Hypothyroidism?
Check the symptoms you experience chronically (most days for 3+ months):
- Persistent fatigue despite adequate sleep
- Unexplained weight gain or inability to lose weight
- Cold hands and feet, feeling cold when others are comfortable
- Hair loss or thinning (including eyebrows)
- Depression, anxiety, or mood changes
- Brain fog, poor concentration, or memory problems
- Constipation
- Dry skin
- Muscle weakness or joint pain
- Heavy or irregular periods (women)
- Low libido or erectile dysfunction (men)
- Slow heart rate
- Puffy face or swollen neck
If you checked 3 or more symptoms: Order comprehensive thyroid testing today.
If you checked 5 or more symptoms: Your thyroid almost certainly needs evaluation.
What Separates “Normal” from Hypothyroid
Hypothyroid sufferers will experience several or many of these symptoms:
- At the same time (not just one symptom in isolation)
- Chronically (not just for a few days or weeks)
- Progressively worsening over time as metabolism slows
Important note: Historically, hypothyroidism has been difficult to diagnose in people over 60, mainly for two reasons:
- Symptoms are often mistaken for “normal aging”
- Frequency of multiple symptoms decreases in older patients (they may have fewer simultaneous symptoms)
This doesn’t mean older adults don’t have hypothyroidism—it just means doctors miss it more often.
The Complete List of Hypothyroidism Symptoms
1. Lethargy: Tiredness Is a State of Being
Lethargy is usually a mode of existence for people with hypothyroidism.
This isn’t “I’m tired today” fatigue. This is:
- Chronic fatigue (very common) – exhaustion that doesn’t improve with rest
- Being able to sleep all the time (common) – could literally nap 24/7
- Constantly feeling heavy and tired (common) – like gravity increased by 50%
- Crippling weariness (uncommon but devastating) – barely functional
The typical hypothyroidism flavor of lethargy translates to:
- Being able to fall asleep on command (give me 30 seconds and a horizontal surface)
- Waking up feeling unrested (even after 10 hours of sleep)
- Feeling extremely tired after only moderate activity (walking up stairs = exhausting)
This fatigue isn’t laziness. It’s cellular dysfunction.
2. Chilliness: More Sweaters Than Shirts in Your Closet
Your thyroid helps regulate internal temperature. When it doesn’t work, your internal thermostat drops.
Many websites claim “sensitivity to cold” as a primary symptom. But this is like saying frostbite is “inconvenient.” With hypothyroidism it’s more like:
- Always having cold hands and feet (my wife refers to my feet as “ice blocks”)
- Feeling cold in warm environments (wearing a jacket when others are in t-shirts)
- Strong sensitivity to cold (winter becomes genuinely unbearable)
You’re not being dramatic. Your body literally cannot maintain normal temperature.
3. Weight Gain: Hypothyroid Is the Only Demographic No Diet Works On
Your thyroid hormone (T3 and T4) regulates metabolism. Without adequate hormone, your metabolism can slow to a point that makes glaciers look hasty.
This explains why people with hypothyroidism:
- Put on weight no matter what they eat (eating 1,200 calories and still gaining)
- Can’t lose a single pound despite diet and exercise (beyond frustrating)
- Feel blamed and shamed for weight they cannot control (the worst part)
This isn’t about willpower or self-control. It’s metabolic dysfunction.
The Hypothyroid Metabolism Reality
| Normal Metabolism | Hypothyroid Metabolism |
|---|---|
| Burns 1,800-2,200 calories daily at rest | May burn only 1,200-1,400 calories daily |
| Responds predictably to calorie reduction | Barely responds to severe restriction |
| Weight loss achievable with modest deficit | Weight loss nearly impossible |
| Exercise increases metabolic rate | Exercise barely moves the needle |
| Food converts to energy efficiently | Food preferentially stored as fat |
You could eat nothing but celery and run marathons, and your body would still struggle to lose weight without adequate thyroid hormone. The metabolism simply isn’t functioning.
If you’re doing everything “right” and still gaining weight, test your thyroid immediately.
4. Paresthesia: That “Pins and Needles” Feeling
Paresthesia is the clinical term for that numb/tingly/pins and needles feeling in your hands or feet for no apparent reason.
With hypothyroidism, this happens because:
- Nerve function is impaired
- Circulation is reduced
- Metabolic processes slow down
If your hands and feet constantly feel like they “fell asleep,” hypothyroidism might be the culprit.
5. Hair Loss: Professional Drain Clogger
The T4 hormone moderates hair cycles and other hair biology. Without adequate T4, your hair is directly affected.
No kidding—this symptom is often a tipoff for many undiagnosed hypothyroid victims and is a sincere concern for people with diagnosed hypothyroidism.
The symptoms look like this:
- Shower drain becomes increasingly clogged (every shower removes alarming amounts)
- Excessive hair when brushing (sometimes in clumps)
- “Empty” patches on your head where scalp shows through
- Thinning on the outer sides of eyebrows (classic hypothyroid sign)
- Overall thinning and brittleness (hair texture changes)
Ladies: This is devastating. Gentlemen: Also devastating, just less socially acceptable to talk about.
6. Abnormal Menstrual Cycle (Women): Getting Pregnant Seems Impossible
Becoming pregnant or staying pregnant can be a major source of frustration and pain for subclinical hypothyroid sufferers.
There’s ongoing debate about whether thyroid screening should be mandatory during pregnancy. The correlation between pregnancy troubles and hypothyroid is strong enough that the American Thyroid Association has issued multiple statements warning about the dangers.
Increased complications include:
- Miscarriage
- Stillbirth
- Infertility
- Anemia
- Preeclampsia
- Placental abruption
- Premature delivery
- Developmental issues in baby
The good news: With proper treatment and monitoring, hypothyroid women often achieve completely normal pregnancies. (My wife with Hashimoto’s had a wonderful pregnancy.)
If you’re struggling with fertility or pregnancy complications, demand thyroid testing.
7. Erectile Dysfunction (Men): Casanova Wasn’t Hypothyroid
Hypothyroidism can cause erectile dysfunction in men through multiple mechanisms:
- Reduced metabolism and energy
- Hormonal imbalances
- Decreased blood flow
- Depression and low mood (which affects libido)
This isn’t “performance anxiety”—it’s a metabolic issue with a medical solution.
8. Depression: When Your Brain Chemistry Is Literally Off
Hypothyroidism and depression have an extremely strong correlation. T3 affects neurotransmitter production, including:
- Serotonin (mood regulation)
- Dopamine (motivation and reward)
- Norepinephrine (energy and focus)
Without adequate thyroid hormone, your brain chemistry is literally malfunctioning.
The Antidepressant That Doesn’t Work
Many people are prescribed antidepressants when the real problem is hypothyroidism. The antidepressants don’t work (or work poorly) because they’re treating a symptom, not the root cause.
Sarah’s Story (Real Patient, Name Changed):
“I was on three different antidepressants over two years. Nothing helped. My psychiatrist kept increasing doses and switching medications. I felt like a failure. Then a new doctor tested my thyroid—my TSH was 8.5. Within a month of starting thyroid medication, my depression lifted more than it had in years. The antidepressants had been trying to fix a problem that didn’t exist. My brain wasn’t broken—my thyroid was.”
If antidepressants aren’t working, test your thyroid immediately. You might not have depression—you might have hypothyroidism.
9. Brain Fog: Mental Moosh
Hypothyroidism causes significant cognitive dysfunction:
- Memory problems (forgetting common words, losing train of thought)
- Difficulty concentrating (reading the same paragraph five times)
- Slow processing speed (takes longer to understand things)
- Mental confusion (feeling “fuzzy” or “cloudy”)
This isn’t early-onset dementia—it’s hypothyroidism. And it’s reversible with treatment.
10. Constipation: Everything Slows Down
Your entire digestive system slows with hypothyroidism. This leads to:
- Chronic constipation
- Bloating
- Sluggish digestion
- Feeling uncomfortably full
Your colon is just as affected by low metabolism as the rest of your body.
11. Dry Skin and Brittle Nails
Thyroid hormone affects skin cell turnover and moisture retention. Without it:
- Skin becomes dry and flaky
- Nails become brittle and break easily
- Wounds heal more slowly
- Overall skin texture worsens
12. Muscle Weakness and Joint Pain
Hypothyroidism causes:
- Muscle weakness (especially in larger muscle groups)
- Joint pain and stiffness
- Muscle cramps
- Slow muscle recovery after exercise
You’re not just “out of shape”—your muscles aren’t getting the metabolic support they need.
13. Hoarseness and Swollen Neck
If the thyroid gland itself is enlarged (goiter):
- Voice may become hoarse
- Neck may appear swollen
- Swallowing might feel difficult
If you notice neck swelling, see a doctor immediately for thyroid evaluation.
14. Slowed Heart Rate (Bradycardia)
Hypothyroidism can slow your heart rate below normal, causing:
- Feeling of heart beating slowly or weakly
- Dizziness
- Fatigue (even worse than baseline hypothyroid fatigue)
- Shortness of breath with minimal exertion
Order Comprehensive Thyroid Testing with MyLabsForLife
If you recognize multiple symptoms on this list, it’s time to test your thyroid—today, not next month.
Don’t wait for:
- Months-long waits for doctor appointments
- Insurance approval battles
- Dismissive doctors who say “everything’s fine” when you feel terrible
- Symptoms to get even worse
Take control of your health right now.
MyLabsForLife: Complete Thyroid Testing Without the Runaround
Why Choose MyLabsForLife for Thyroid Testing?
- No Doctor’s Order Required – Order online in 5 minutes, test this week
- Complete Thyroid Panels – TSH, Free T3, Free T4, Reverse T3, Antibodies (all the tests doctors skip)
- Fast Results – 7-10 day turnaround (not weeks or months)
- Affordable Pricing – No insurance markups, surprise bills, or copay games
- CLIA-Certified Labs – Hospital-quality testing (same labs your doctor uses)
- Nationwide Access – Thousands of collection sites across the US
- Educational Resources – Actually understand your results (not just numbers on paper)
- Privacy Guaranteed – Your health data stays confidential
- No Judgment – Test as often as needed to monitor your health
Choose Your Thyroid Testing Panel
Basic Thyroid Panel: The Starting Point
- TSH + Free T4
- Good for initial screening
- Identifies most cases of hypothyroidism
- Best for: First-time testing, budget-conscious screening
Complete Thyroid Panel: The Smart Choice
- TSH, Free T3, Free T4, Reverse T3
- Comprehensive metabolic assessment
- Identifies conversion problems TSH alone misses
- Best for: People with symptoms despite “normal” TSH, comprehensive evaluation
Advanced Thyroid Panel: The Gold Standard
- Everything above PLUS TPO & Thyroglobulin Antibodies
- Detects autoimmune thyroid disease (Hashimoto’s)
- Most complete assessment available
- Best for: Family history of autoimmune disease, unexplained infertility, comprehensive root cause analysis
Order Your Thyroid Panel at MyLabsForLife.com
Most people choose the Complete Panel—it catches problems the Basic panel misses, and costs far less than dealing with years of undiagnosed hypothyroidism.
What Causes Hypothyroidism? Understanding the Root Causes
1. Hashimoto’s Thyroiditis (Autoimmune Disease)
The most common cause of hypothyroidism in developed countries.
Hashimoto’s occurs when your immune system mistakenly attacks your thyroid gland, gradually destroying its ability to produce hormone.
Key points:
- Affects women 7-10 times more than men
- Often runs in families
- Can be triggered by stress, infections, or environmental factors
- Detected by elevated TPO antibodies
2. Iodine Deficiency
Iodine is required for thyroid hormone production. Without adequate iodine, your thyroid cannot make T3 and T4.
However: Iodine deficiency is relatively uncommon in developed countries with iodized salt. But it can occur with:
- Strict diets avoiding iodized salt
- Vegan diets without supplementation
- Certain geographic areas with iodine-depleted soil
3. Thyroid Surgery or Radiation
Removal of part or all of the thyroid (for cancer, nodules, or hyperthyroidism) obviously reduces thyroid hormone production.
Radiation therapy to the neck area can also damage the thyroid.
4. Medications
Certain medications can interfere with thyroid function:
- Lithium (psychiatric medication)
- Amiodarone (heart medication)
- Interferon alpha (immune system medication)
- High-dose biotin (interferes with thyroid testing)
5. Pituitary or Hypothalamus Problems
Less commonly, the problem isn’t with the thyroid itself but with the pituitary gland (not producing enough TSH) or hypothalamus (not producing enough TRH).
This is called secondary or tertiary hypothyroidism and requires different treatment approaches.
Environmental Factors and Thyroid Disruptors
Glyphosate: The Herbicide Destroying Your Thyroid
Glyphosate (the active ingredient in Roundup) is one of the most serious threats to thyroid health in our modern environment.
How glyphosate damages your thyroid:
- Disrupts gut bacteria (which help convert T4 to active T3)
- Acts as an endocrine disruptor
- Chelates essential minerals needed for thyroid function (selenium, zinc)
- Creates chronic inflammation that impairs thyroid function
Glyphosate is in:
- 90% of conventional crops
- Your drinking water (even in cities far from farmland)
- The air in agricultural areas (spray drift travels miles)
- Tampons and cotton products (conventional cotton is heavily sprayed)
- Even in organic food at low levels (through contamination)
Minimize Glyphosate Exposure: Action Steps
Immediate Actions:
- Switch to organic produce (especially high-residue crops: oats, wheat, corn, soy, legumes)
- Filter your water (reverse osmosis or quality carbon filter removes glyphosate)
- Choose organic cotton products (tampons, pads, clothing, bedding)
- Avoid conventional grains (glyphosate is used as a drying agent on wheat, oats)
- Test your exposure levels (MyLabsForLife offers glyphosate testing)
For more information, see our comprehensive article: Glyphosate: Make America Great Again and Stop Spraying
Test your glyphosate exposure with MyLabsForLife to understand if this toxin is contributing to your thyroid dysfunction.
Dioxins: The Agent Orange Component
Dioxin is one wicked dude. It’s the primary toxic component of Agent Orange—enough said.
The damage:
- Half-life in the body: 7-11 years
- Potential thyroid damage: permanent [5]
- Source: By-products of industrial processes (waste centers)
- Entry route: Contaminated food
You can’t easily avoid dioxins, but you can minimize exposure by:
- Choosing organic, grass-fed animal products
- Avoiding high-fat conventional dairy (dioxins concentrate in fat)
- Supporting liver detoxification
Soy: The Controversial Thyroid Disruptor
Believe it or not, excessive soy may disrupt iodine absorption because isoflavone inhibits thyroid peroxidase (TPO)—an enzyme that produces thyroid hormone.
Important nuance:
- Moderate soy consumption in people with adequate iodine intake: probably fine
- High soy consumption in people with borderline iodine: problematic
- Processed soy (soy protein isolate): more concerning than fermented soy
Note: Isoflavone doesn’t seem to inhibit thyroid function in otherwise healthy individuals with adequate iodine intake [see references 61-63].
Pay attention to your risk factors and soy consumption if you have thyroid issues.
Pesticides: Not Just Killing Honeybees
Pesticides aren’t just killing off the world’s honeybees (Google “Neonicotinoids” for a depressing rabbit hole)—they can also hurt thyroid function.
One study found: Women married to men who used pesticides were twice as likely to develop thyroid disease.
Let that sink in. Just being married to someone who uses pesticides doubles your risk.
Minimize exposure by:
- Choosing organic produce (especially high-pesticide items)
- Washing all produce thoroughly
- Avoiding residential pesticide use
- Supporting regenerative agriculture
PFOA: The Teflon Chemical Everywhere
Perfluorooctanoic acid (PFOA) is another evil little chemical, and it’s everywhere:
- Teflon (used in cookware)
- Food wrappers (stores your food)
- Microwave popcorn bags (movie night toxin delivery)
- Waterproof clothing
- Stain-resistant fabrics
The evidence: A large study funded by part of a $100 million settlement with DuPont (over allegedly dumping PFOA in drinking water) concluded that PFOA can affect thyroid function at even modest levels of exposure.
Minimize exposure by:
- Ditching Teflon cookware (use cast iron, stainless steel, ceramic)
- Avoiding microwave popcorn
- Filtering drinking water with quality carbon filter or reverse osmosis
- Choosing natural fiber products
Triclosan: The Antibacterial Thyroid Killer
Check the ingredients on your:
- Soap
- Lotion
- Toothpaste
Triclosan is an antibacterial chemical that not only kills bad bugs but may significantly impact thyroid hormone levels.
The FDA banned triclosan from soaps in 2016, but it’s still in many products.
Avoid products listing triclosan in ingredients.
Thyroid Hormone Testing and Diagnosis
In general, diagnosing hypothyroidism is fairly straightforward—if you order the right tests.
In the past, basal body temperature was used to aid diagnosis. Currently, there are several tests to assess thyroid function, and they should be used in conjunction, not alone. Be sure your are working with a qualified health care provider. Thyroid hormone is nothing to mess around with!
The Hallmark of Hypothyroidism Diagnosis
One or a combination of:
- High TSH levels (pituitary stepping on gas pedal)
- Low T4 and T3 levels (inadequate hormone production)
- High Reverse T3 levels (inactive hormone blocking receptors)
- High antibodies (autoimmune attack on thyroid)
Complete Thyroid Panel Test: What You Need
A Thyroid Panel is a combination of the main tests for thyroid disease:
- TSH test
- Free T4 test
- Free T3 test
- Reverse T3 test
- Thyroid Peroxidase Antibodies (TPO) test
- Thyroglobulin Antibodies test
This comprehensive panel should almost always be used to diagnose thyroid disease. TSH alone is insufficient.
1. TSH Test (Thyroid Stimulating Hormone)
What it measures: How much TSH your pituitary is producing
What it means:
- High TSH = Low thyroid hormone (hypothyroidism) – pituitary pressing hard on gas pedal
- Low TSH = High thyroid hormone (hyperthyroidism) – pituitary letting off gas pedal
Important: TSH alone doesn’t tell the whole story. You need the complete panel.
See our detailed article: What Is TSH and Why It Matters
2. Free T4 Test (Thyroxine)
What it measures: Thyroxine levels (main thyroid hormone)
What it means:
- Low T4 causes trademark hypothyroid symptoms: depression, weight gain, hair loss, cold intolerance
- Free T4 is the unbound, bioavailable form
See our detailed article: T4 Test Overview
3. Free T3 Test (Triiodothyronine)
What it measures: Active thyroid hormone levels
What it means:
- T3 is the “active” version of T4
- Converted from T4 by iodine and friendly gut bacteria
- Affects almost every physiological process: growth, development, metabolism, body temperature, heart rate
Critical point: You can have normal TSH and T4 but low T3 (conversion problem). This explains why some people have all the symptoms but “normal” labs.
4. Reverse T3 Test (rT3)
What it measures: Inactive T3 levels
What it means:
- With normal thyroid, about 20% of T4 converts to T3
- The rest becomes Reverse T3 (inactive form)
- rT3 blocks T3 receptors (acts as brake on thyroid function)
- Your body recognizes rT3 as T3, so it stops making more
High Reverse T3 indicates:
- Chronic stress
- Inflammation
- Illness or infection
- Nutrient deficiencies
- Heavy metal toxicity
This is why you can have “normal” thyroid tests but feel hypothyroid.
5. Thyroid Antibody Tests (TPO and Thyroglobulin)
What they measure: Immune system attack on thyroid
TPO (Thyroid Peroxidase Antibodies):
- Tests if antibodies are attacking the enzyme that makes thyroid hormone
- Positive = Hashimoto’s thyroiditis (autoimmune hypothyroidism)
- Can be elevated years before TSH becomes abnormal
Thyroglobulin Antibodies:
- Tests if antibodies are attacking thyroid hormone itself
- May lead to thyroid destruction
- Also associated with Hashimoto’s
Why this matters: If you have positive antibodies, you need a different treatment approach that addresses the autoimmune component, not just hormone replacement.
Order Your Complete Thyroid Panel Today
Stop settling for incomplete testing that misses the root cause.
Order Complete Thyroid Testing at MyLabsForLife.com
MyLabsForLife offers all the tests doctors often skip:
- Full thyroid panel with all markers
- No need to convince your doctor to order tests
- No insurance denials or fighting for coverage
- Fast results you can understand
- Resources to interpret your results
Treatment for Hypothyroidism: Conventional and Functional Approaches
Conventional Treatment: Hormone Replacement
When diagnosis is confirmed, the most common treatment is thyroid hormone replacement. The goal is to relieve symptoms and decrease elevated TSH to normal range.
Typical treatments begin with:
Synthetic T4 (Levothyroxine):
- Brand names: Synthroid, Levoxyl, Tirosint
- Replaces T4 hormone
- Requires conversion to active T3
- Most commonly prescribed
Dosing strategy:
- Generally, low doses given initially
- Slowly increased until hormone levels are in healthy range
- Requires regular monitoring and adjustments
Timing tip: A 2009 paper suggests it’s more effective to take thyroid medication just before bed rather than in the morning (though many doctors still recommend morning dosing).
When T4-Only Isn’t Enough
Some people don’t convert T4 to T3 efficiently. For these patients:
T3 medication options:
- Liothyronine (synthetic T3)
- Combination T4/T3 medications
- Natural desiccated thyroid (NDT) – contains both T4 and T3
Work with a knowledgeable practitioner to determine if you need T3 supplementation.
Functional Medicine Approach: Address Root Causes
Beyond conventional hormone replacement, functional medicine addresses:
1. Autoimmunity (if Hashimoto’s)
- Reduce inflammation
- Identify food triggers (often gluten, dairy)
- Support immune system regulation
- Address gut health
2. Nutrient Deficiencies
- Test and optimize thyroid-supporting nutrients
- Supplement strategically
- Address malabsorption issues
3. Environmental Toxins
- Reduce glyphosate exposure
- Minimize endocrine disruptors
- Support detoxification pathways
4. Gut Health
- Heal leaky gut
- Restore healthy microbiome
- Optimize T4 to T3 conversion
5. Stress Management
- Reduce cortisol (which increases Reverse T3)
- Support adrenal function
- Improve sleep quality
Supporting a Healthy Thyroid: Essential Nutrients
The following minerals and vitamins are extremely important—if not essential—to healthy thyroid function:
Critical Thyroid Nutrients
Iodine:
- Required for T4 and T3 production
- Deficiency causes hypothyroidism
- Too much can also cause problems (moderation)
Selenium:
- Required for converting T4 to active T3
- Protects thyroid from oxidative damage
- Deficiency common in many regions
Zinc:
- Needed for thyroid hormone production
- Required for T4 to T3 conversion
- Deficiency very common
Iron:
- Required for thyroid peroxidase activity
- Deficiency impairs thyroid function
- Women particularly at risk
Copper:
- Balances zinc (they work together)
- Needed for thyroid hormone production
Vitamin E:
- Antioxidant protection for thyroid
- Supports hormone production
Vitamin D:
- Immune system regulation (critical for Hashimoto’s)
- Often deficient in hypothyroid patients
Vitamin B12:
- Energy production
- Often low in hypothyroid patients
- Supports nerve function
For detailed information on why these nutrients are essential and how to optimize them, see our comprehensive guide: Essential Nutrients for Thyroid Health
Test Your Thyroid and Nutrient Levels with MyLabsForLife
You can’t optimize what you don’t measure.
MyLabsForLife offers comprehensive testing panels:
- Complete thyroid panels (TSH, Free T3, Free T4, Reverse T3, antibodies)
- Nutrient testing (vitamin D, B12, iron, selenium, zinc)
- Metabolic panels
- And much more
Order Your Testing Panel at MyLabsForLife.com
Frequently Asked Questions About Hypothyroidism
Q: Can hypothyroidism be cured? A: It depends on the cause. Hashimoto’s and surgical removal are typically permanent, requiring lifelong hormone replacement. Some cases of subclinical hypothyroidism can be reversed with lifestyle changes and nutrient optimization.
Q: How long does it take to feel better after starting treatment? A: Most people notice improvement within 2-4 weeks of starting medication. Full optimization can take 3-6 months as dosage is adjusted and lifestyle changes take effect.
Q: Will I gain weight from thyroid medication? A: No—the opposite. Proper thyroid hormone replacement should help normalize metabolism and make weight loss possible again (though it’s not automatic).
Q: Can I stop thyroid medication once I feel better? A: Generally no. Most people need lifelong hormone replacement. Never stop medication without consulting your healthcare provider.
Q: Is hypothyroidism hereditary? A: Yes, thyroid disease runs in families. If you have a family history, you should be screened regularly.
Q: Can stress cause hypothyroidism? A: Chronic stress can trigger or worsen hypothyroidism, especially autoimmune forms like Hashimoto’s. Stress also increases Reverse T3, making existing hypothyroidism worse.
Q: Should I avoid gluten if I have hypothyroidism? A: If you have Hashimoto’s (autoimmune hypothyroidism), gluten elimination often helps reduce antibodies and inflammation. If you don’t have Hashimoto’s, gluten may not be an issue (test to find out).
Q: Can I have hypothyroidism with normal TSH? A: YES. This is common when you have conversion problems (low T3 despite normal TSH and T4) or high Reverse T3. This is why complete thyroid panels are essential.
Q: How often should I retest my thyroid? A: When starting treatment: every 6-8 weeks until stable. Once optimized: every 6-12 months. If symptoms return: immediately.
Take Control of Your Thyroid Health Today—Don’t Wait Another Day
If you recognize multiple symptoms on this list, don’t wait.
10 million Americans are walking around undiagnosed, feeling terrible, being told “everything’s normal,” and suffering unnecessarily.
Don’t be another statistic.
Your Next Steps (Take Action Today)
Step 1: Order Comprehensive Thyroid Testing (5 minutes) Get the complete picture with TSH, Free T3, Free T4, Reverse T3, and antibodies through MyLabsForLife. No doctor’s order needed. No insurance hassles.
Step 2: Review Your Results (7-10 days) MyLabsForLife provides clear explanations, reference ranges, and optimal targets—not just numbers you don’t understand. Always review with your trusted health care provider.
Step 3: Take Results to Healthcare Provider (or find a new one) Find someone who understands functional thyroid treatment, not just TSH normalization. If your current doctor dismisses your symptoms, find a provider who won’t.
Step 4: Begin Treatment and Lifestyle Modifications Address hormone replacement AND root causes. Optimal health requires both.
Step 5: Retest Regularly (Monitor progress) Track improvements and adjust treatment as needed. MyLabsForLife makes ongoing monitoring affordable.
What Happens If You Don’t Test?
Let’s be blunt about what untreated hypothyroidism looks like:
- Years of unnecessary suffering (fatigue, depression, weight gain that won’t budge)
- Worsening symptoms (hypothyroidism is progressive—it doesn’t improve on its own)
- Fertility problems (unexplained infertility, miscarriages, complications)
- Cardiovascular damage (elevated cholesterol, increased heart disease risk)
- Cognitive decline (brain fog that worsens over time)
- Metabolic syndrome (weight gain, insulin resistance, diabetes risk)
- Quality of life destruction (relationships suffer, career suffers, parenting suffers)
Or you could test now and potentially feel dramatically better within weeks.
The choice is obvious.
Order Your Complete Thyroid Panel Now
Your thyroid controls every cell in your body. When it fails, everything suffers.
Get Started at MyLabsForLife.com
Questions? MyLabsForLife’s customer support team is ready to help you choose the right panel and understand your results.
Share this guide with anyone struggling with unexplained fatigue, weight gain, depression, or other mysterious symptoms. It might change their life.
Your path to enhanced cellular wellness starts with understanding your thyroid—and that starts with comprehensive testing.
Health Disclaimer & Legal Information
Medical Disclaimer:
The statements on this site have not been evaluated by the Food and Drug Administration. Any health education or products mentioned or discussed on this site are not intended to diagnose, treat, cure, or prevent any disease. The information on this site is not intended to be a substitute for professional medical advice.
Important Notes:
It is recommended the reader of this site consult with a qualified health care provider of their choice when using any information obtained from this site, affiliate sites, and other online websites and blogs. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition.
The health-related and medical information on this site is provided as an information resource only, and is not to be used or relied on for any diagnostic or treatment purposes. This information is not intended to be patient education, does not create any patient-physician, client-nurse practitioner, or patient-pharmacist relationship, and should not be used as a substitute for professional diagnosis and treatment.
Service Information:
You understand the service provided by My Labs For Life, LLC is a service provided at your request and not suggested by our medical director or education staff.
Evidence-Based and Theoretical Information:
In concert with evidence-based information, this site proposes certain theoretical methods of functional and nutritional support that may not be supported by conventional or mainstream medicine. Any information obtained from this site is left to the discretion and is the sole responsibility of the user of this site.
Liability Waiver:
The contributors of this site cannot be held responsible for the information or any inadvertent errors or omissions of the information. By visiting this site you agree to the foregoing terms and conditions, which may be changed or supplemented at any time. If you do not agree to the foregoing terms and conditions, you should not enter this site.
The contributors of this site shall have no liability for any damages, loss, injury, or liability whatsoever suffered as a result of your reliance on the information contained in this site.
References & Scientific Citations
[1] American Association of Clinical Endocrinologists. (2023). Thyroid Disease Statistics and Awareness.
[2] Cheng, S.Y., Leonard, J.L., & Davis, P.J. (2010). Molecular aspects of thyroid hormone actions. Endocrine Reviews, 31(2), 139-170.
[3] Garber, J.R., et al. (2012). Clinical practice guidelines for hypothyroidism in adults. Endocrine Practice, 18(6), 988-1028.
[4] Zimmermann, M.B., & Boelaert, K. (2015). Iodine deficiency and thyroid disorders. The Lancet Diabetes & Endocrinology, 3(4), 286-295.
[5] Langer, P., et al. (2007). Persistent organochlorinated pollutants and thyroid function. Molecular and Cellular Endocrinology, 265-266, 178-181.
Additional References:
- Myers, A. (2016). The Thyroid Connection. Little, Brown Spark.
- Duntas, L.H., & Benvenga, S. (2015). Selenium: an element for life. Endocrine, 48(3), 756-775.
- Triggiani, V., et al. (2009). Role of iodine, selenium and other micronutrients in thyroid function and disorders. Endocrine, Metabolic & Immune Disorders Drug Targets, 9(3), 277-294.
Ready to understand your thyroid? Order your complete panel from MyLabsForLife now.
Because 10 million undiagnosed Americans deserve better.
Your thyroid controls everything. Time to find out if it’s working.
Additional Resources
Check out our bookstore on MyLabsForLife for recommended reading on thyroid health, functional medicine, and cellular wellness: https://mylabsforlife.com/book-store/
Need high-quality vitamins and supplements to support your thyroid health? Visit our Fullscript store via QualityVitaminStore.com: https://qualityvitaminstore.com/